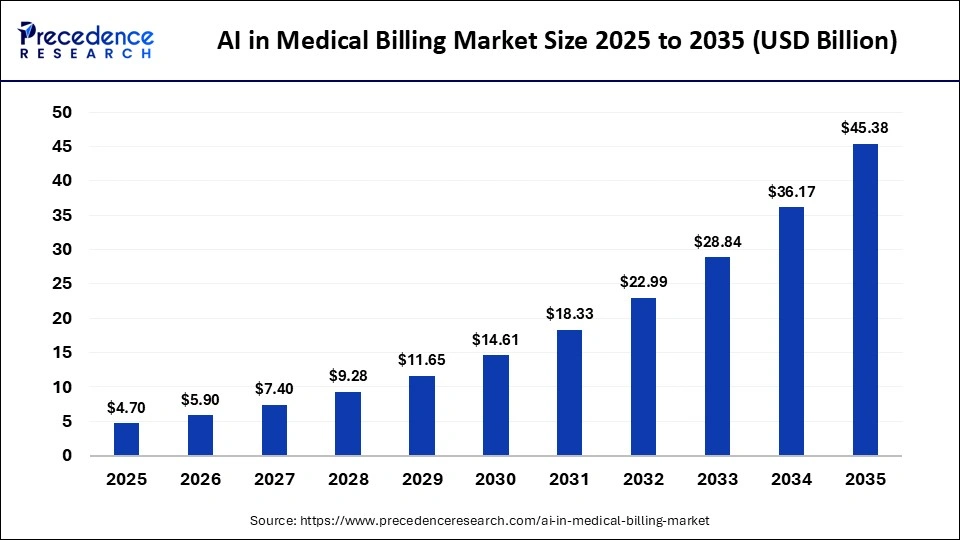
What is the AI in Medical Billing Market Size in 2026?
The global AI in medical billing market is experiencing rapid transformation, driven by the increasing digitization of healthcare systems and the growing need for efficient financial operations. The market size was valued at USD 4.70 billion in 2025 and is projected to grow from USD 5.90 billion in 2026 to approximately USD 45.38 billion by 2035, expanding at an impressive CAGR of 25.44% during the forecast period.
This exponential growth is fueled by the rising demand for automation in revenue cycle management (RCM), increasing healthcare data volumes, and the need to minimize billing errors while accelerating claims processing.
Read Also: Neurorehabilitation Devices Market
Market Overview
AI in medical billing refers to the application of advanced technologies such as machine learning (ML), natural language processing (NLP), robotic process automation (RPA), and predictive analytics to streamline billing workflows. These solutions automate tasks like medical coding, claim submission, denial management, and payment processing.
Healthcare providers are increasingly adopting AI-powered billing systems to:
- Reduce administrative burden
- Improve coding accuracy
- Accelerate reimbursements
- Enhance compliance with regulations
- Optimize overall financial performance
The integration of AI into billing processes is transforming traditional systems into intelligent, adaptive, and data-driven ecosystems.
Key Market Highlights
- North America dominated the market with a 41% share in 2025
- Asia-Pacific is projected to grow at the fastest rate
- AI software platforms held the largest share (46%)
- Cloud-based deployment dominated with 63% share
- Machine learning led technology adoption (41% share)
- Hospitals and clinics accounted for 56% of total demand
Role of AI in Medical Billing
Artificial intelligence plays a crucial role in modernizing healthcare billing operations. AI systems can process vast amounts of structured and unstructured data, ensuring faster and more accurate billing cycles.
Key AI Capabilities:
- Automated medical coding: NLP extracts information from clinical notes
- Denial prediction: ML models identify claims likely to be rejected
- Fraud detection: AI identifies anomalies and compliance issues
- Real-time claim validation: Immediate error detection before submission
- Revenue optimization: Predictive analytics reduces revenue leakage
AI-driven platforms continuously learn from past billing data, improving efficiency and reducing manual intervention over time.
Technology Advancements Shaping the Market
The AI in medical billing market is evolving with several technological innovations:
- Transformer-based NLP models for accurate clinical data extraction
- Closed-loop learning systems that improve from claim outcomes
- API-driven ecosystems enabling seamless integration with EHR systems
- Real-time processing engines for instant billing validation
- Unsupervised learning models for anomaly and fraud detection
These advancements are making billing systems more intelligent, scalable, and adaptive.
Market Trends
1. Rising Strategic Collaborations
Healthcare IT firms and AI providers are forming partnerships to develop integrated billing solutions. These collaborations combine domain expertise with advanced analytics to improve efficiency.
2. Government Digital Health Initiatives
Government programs promoting electronic health records and digital infrastructure are accelerating AI adoption in billing systems.
3. Expansion of AI-Driven RCM Platforms
Companies are expanding from basic billing tools to comprehensive revenue cycle management platforms powered by AI.
4. Increasing Use of Predictive Analytics
Healthcare providers are leveraging predictive tools to anticipate claim denials and optimize submission strategies.
Segmental Insights
By Offering Type
AI Software Platforms dominated the market in 2025 due to their ability to provide end-to-end automation. These platforms integrate coding, claims processing, and analytics into a single system.
Data Analytics and Optimization Tools are expected to grow at the fastest rate, as healthcare organizations increasingly rely on data-driven insights to improve financial performance.
By Deployment Type
Cloud-Based Platforms led the market with a 63% share due to:
- Scalability
- Cost efficiency
- Remote accessibility
- Seamless integration
Hybrid Deployments are gaining traction as they offer a balance between data security and scalability.
By Technology Type
Machine Learning dominated the market, enabling:
- Pattern recognition in claims data
- Automated error detection
- Continuous system improvement
Predictive Analytics is expected to grow rapidly, helping organizations forecast denials and optimize revenue cycles.
By End User
Hospitals and Clinics held the largest share due to complex billing processes and high claim volumes.
Billing Outsourcing Firms are expected to witness the fastest growth, as they adopt AI to handle large-scale operations efficiently.
Regional Insights
North America
North America remains the dominant region due to:
- Advanced healthcare infrastructure
- High adoption of AI technologies
- Complex insurance and billing systems
The United States leads the region with strong investments in healthcare IT and revenue cycle innovations.
Asia-Pacific
Asia-Pacific is expected to grow at the fastest CAGR due to:
- Rapid healthcare digitization
- Growing patient population
- Increased adoption of cloud-based systems
Countries like China and India are emerging as key markets due to expanding healthcare infrastructure and AI adoption.
Europe
Europe is witnessing steady growth driven by:
- Regulatory compliance requirements
- Adoption of digital health systems
- Government-supported healthcare initiatives
Competitive Landscape
Key companies operating in the AI in medical billing market include:
- Waystar
- NextGen Healthcare, Inc.
- McKesson Corporation
- Epic Systems Corporation
- Athenahealth, Inc.
- eClinicalWorks LLC
- GE Healthcare
- Optum, Inc.
- RapidClaims.Ai
- Nym Health
These companies are focusing on AI integration, partnerships, and product innovation to strengthen their market position.
Recent Developments
- Jorie AI (2025): Introduced SmartCore Engine for intelligent billing automation
- Azalea Health (2025): Launched AI Billing Assistant to reduce coding errors
- Cedar (2025): Developed AI voice agent “Kora” for patient billing support
Future Outlook
The future of the AI in medical billing market looks highly promising, with increasing reliance on automation and intelligent systems. As healthcare systems continue to digitize, AI will play a central role in reducing administrative costs, improving billing accuracy, and enhancing patient experience.
Emerging technologies such as generative AI, real-time analytics, and autonomous billing systems are expected to further revolutionize the industry.
Conclusion
The AI in medical billing market is undergoing rapid transformation, driven by technological advancements and the growing need for efficient healthcare financial systems. With a projected market size of USD 45.38 billion by 2035, the industry is set to witness substantial growth.
Organizations that invest in AI-powered billing solutions will gain a competitive advantage by improving operational efficiency, reducing errors, and maximizing revenue outcomes.
Get Sample Copy: https://www.precedenceresearch.com/sample/7918
For inquiries regarding discounts, bulk purchases, or customization requests, please contact us at sales@precedenceresearch.com